A 46-year old healthy male is admitted to the ICU for respiratory failure secondary to COVID-19 pneumonia. He is mechanically ventilated for 4 days until he successfully passes a spontaneous breathing trial and is extubated. He is then placed on high flow nasal cannula and is weaned to low flow nasal cannula later that day. Three days post-extubation he develops a new increased oxygen requirement, tachycardia and remains normotensive. A point of care ultrasound of the heart and lungs below is performed.
What do the images show? What is the diagnosis? (Click the button for the answer!)

COVID-19 Pneumonia, Pulmonary Embolism
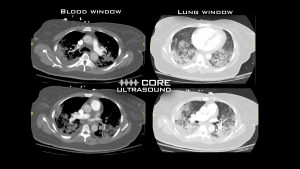
Evidence of subpleural consolidation with pleural irregularities are seen on the bilateral lung ultrasound. There are significant B-lines, consistent with COVID-19 infection.1
The apical 4-chamber view shows enlargement of the right ventricle relative to the left ventricle, which implies right heart dysfunction. This should increase suspicion for an acute pulmonary embolism in the right clinical setting.2
Besides looking for right heart enlargement there are other calculations that can be performed to assess for right heart dysfunction. For a tutorial on right heart dysfunction, Click here
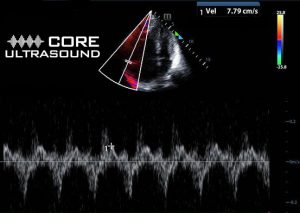
The systolic excursion velocity (S’) is a measure of RV dysfunction and is obtained by placing pulsed tissue Doppler over the lateral aspect of the tricuspid annulus. Normal values are >10cm/s. In our patient, S’ is found to be 7.8cm/s, consistent with decreased RV function.3
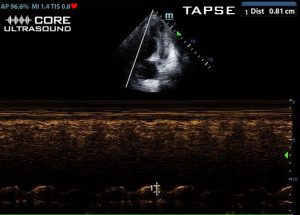
A TAPSE, or tricuspid annular plane systolic excursion, is measured by placing the M-mode cursor on the lateral annulus of the tricuspid valve. A normal value is >20mm with a reduced value being <17mm. Our patient has a TAPSE of 8.1 mm, which is abnormally reduced. A reduced value is associated with decreased systolic function, but not necessarily acute.3
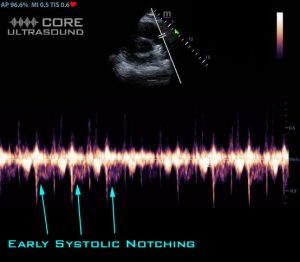
Pulse wave doppler is aligned through the RV outflow tract with two subsequent findings. First, a notable pattern is seen which is known as early systolic notching. This is one of the more specific findings of acute pulmonary embolism.4
The case concludes that the patient had enough evidence of acute pulmonary embolism with right heart strain to begin empiric anticoagulation while waiting on CT scan to be performed. The scan was ultimately performed 36 hours later demonstrating bilateral pulmonary emboli.
- In the right clinical context, point of care ultrasound can quickly raise or lower your suspicion for acute pulmonary embolism.2
- In the COVID population, point of care ultrasound is particularly useful while waiting on confirmatory testing
- Early systolic notching was recently described as one of the best indicators of acute submassive or massive PE with a positive predictive value of 94%.4
- In the same study, the 60/60 sign performed nearly as well with a positive predictive value of 92%.4
To learn more about COVID-associated thrombosis, check out our summary page
Case Courtesy of Terren Trott, MD
Peer Reviewed by Jacob Avila, MD
References
-
- Buonsenso D, Piano A, Raffaelli F, Bonadia N, de Gaetano Donati K, Franceschi F. Point-of-Care Lung Ultrasound findings in novel coronavirus disease-19 pnemoniae: a case report and potential applications during COVID-19 outbreak. European review for medical and pharmacological sciences. 2020; 24(5):2776-2780. [PMID: 32196627]
- Matthews JC, McLaughlin V. Acute right ventricular failure in the setting of acute pulmonary embolism or chronic pulmonary hypertension: a detailed review of the pathophysiology, diagnosis, and management. Current cardiology reviews. 2008; 4(1):49-59. [PMID: 19924277]
- Rudski LG, Lai WW, Afilalo J. Guidelines for the echocardiographic assessment of the right heart in adults: a report from the American Society of Echocardiography endorsed by the European Association of Echocardiography, a registered branch of the European Society of Cardiology, and the Canadian Society of Echocardiography. Journal of the American Society of Echocardiography : official publication of the American Society of Echocardiography. 2010; 23(7):685-713; quiz 786-8. [PMID: 20620859]
- Afonso L, Sood A, Akintoye E. A Doppler Echocardiographic Pulmonary Flow Marker of Massive or Submassive Acute Pulmonary Embolus. Journal of the American Society of Echocardiography : official publication of the American Society of Echocardiography. 2019; 32(7):799-806. [PMID: 31056367]


