Answer: Mitral Inflow Velocity Variation
This echocardiogram demonstrates a large, loculated pericardial effusion, known to be chronic in this patient. The IVC is plethoric, suggesting a high CVP. Without adequate views of the right heart, visualization of the classically described right ventricular diastolic collapse is not possible.1 Furthermore, in a patient with HIV there are a number of potential causes of hypotension.
 Respiratory-phasic changes in mitral inflow velocity is sensitive for tamponade physiology, and is the echo equivalent of pulsus paradoxus.
Respiratory-phasic changes in mitral inflow velocity is sensitive for tamponade physiology, and is the echo equivalent of pulsus paradoxus.- Mitral inflow velocity can be measured in this way: obtain an apical view of the heart, place the pulse wave marker just past the tip of the mitral leaflets (see diagram), then hit the pulse wave button.
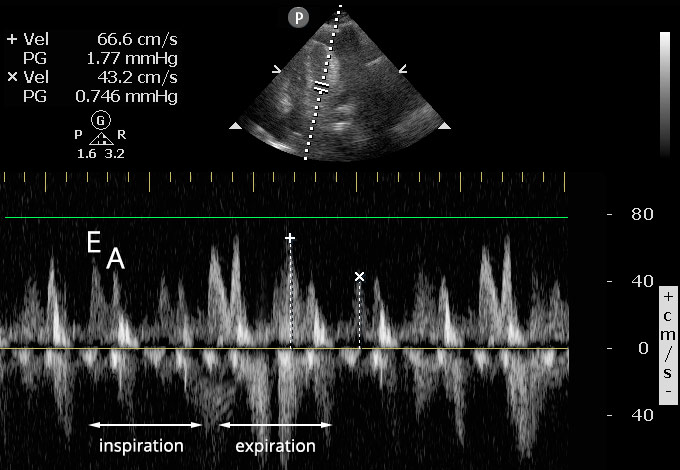
- The image produced plots the velocity of blood flow vs time. The inflow velocities are above the baseline, where you will typically see an E spike and an A spike (labeled below).
- The largest and smallest E spikes should be measured, corresponding to mitral inflow during inspiration and expiration. A variation of 25% or more in the mitral inflow velocity supports a diagnosis of tamponade physiology.1
- It is important to note that mitral inflow variation should be taken within the patients clinical context. It will also be positive when there are wide swings in intrathoracic pressure (COPD) and in other conditions such as pulmonary embolism and hypovolemic shock.2 Vena caval respiratory-phasic changes can effectively rule out tamponade, making hypovolemic shock a more likely culprit.3
- Tricuspid inflow velocity variation can be measured in much the same way as mitral inflow velocity, a tricuspid variation of 40% corresponds to pulsus paradoxus.1
- Measurement of mitral inflow velocity is useful in other clinical scenarios as well: to assess for diastolic heart failure, and to assess for volume responsiveness.
- Otto CM. Textbook of Clinical Echocardiography, Expert Consult – Online and Print. Elsevier Health Sciences; 2013. [amazon]
- Little WC, Freeman GL. Pericardial disease. Circulation. 2006;113(12):1622-32. [PDF]
- Himelman RB, Kircher B, Rockey DC, Schiller NB. Inferior vena cava plethora with blunted respiratory response: a sensitive echocardiographic sign of cardiac tamponade. J Am Coll Cardiol 1988;12: 1470–7. [pubmed]



